Safer, Faster, Clearer Imaging.
What if we adapted the imaging equipment to the moving patient, rather than making the patient conform to the limitations of the equipment? Acquiring images only when the heart and lungs are in perfect position would result in clearer images, and no unnecessary radiation dose to the patient.
We’re creating imaging protocol software that connects the imaging equipment to motion signals taken from the patient (e.g. breathing and the heart beating). By syncing the machine to the patient, we can ensure images are taken at the exact moments when there will be minimal potential for blurring or artefacts.
In Patient Connected Imaging, the patient’s ECG signal is utilized by our software to control the scanner, only collecting images at precise points in the ECG. All images collected are used, significantly reducing the imaging radiation dose.
Team Contact
For more information about the program and projects, contact Dr Tess Reynolds
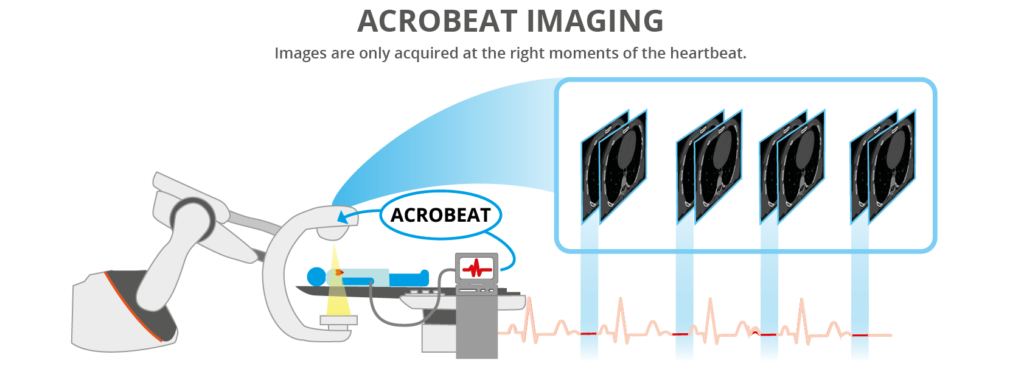
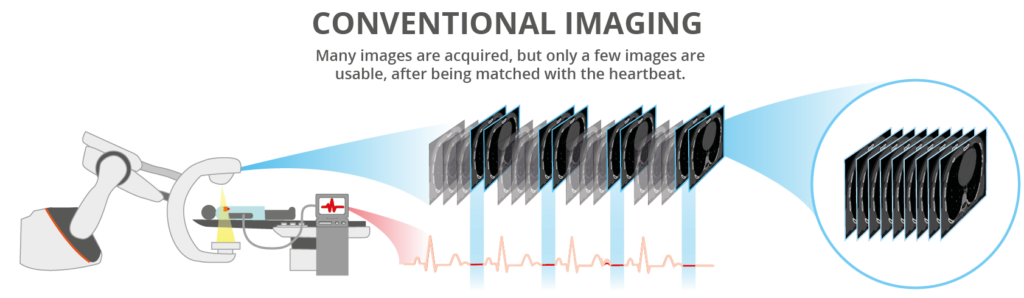
Comparison
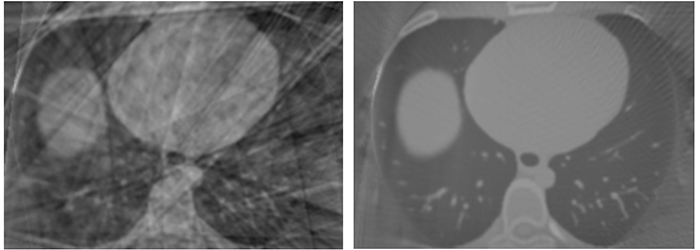
(left) Example of conventional robotic C-arm retrospective ECG gated acquisition (right) ACROBEAT acquisition
How does ACROBEAT Work?
ACROBEAT is a type of ‘imaging protocol’. Medical imaging systems have multiple protocols, – each for use in different scenarios. A helpful analogy is a Digital SLR Camera, with its different settings (protocols) for photographing portraits, landscapes, macro, indoor or outdoor scenes. Where a Digital SLR camera’s protocols/settings optomise the camera to photograph in different situations such as sport, portrait or landscape, the protocols for medical imaging might include the strength of the x-ray, the rotation speed of the gantry, the duration of the scan etc.
ACROBEAT utilizes two additional elements not currently used in conventional image acquisition protocols: the velocity of the gantry that rotates around the patient, and the time interval between each image (projection) being taken. These are the elements that are adapted by the patient’s respiratory trace, ECG or both in real-time.

Respiratory and cardiac signals (red & blue) inform when the projections (yellow) are taken, as the imaging equipment rotates around the patient.
Current Status
In 2021, ACROBEAT was implemented on a clinical robotic imager for the first time, enabling 40% improvement in image quality with a 90% reduction in imaging dose compared to current imaging techniques.
Journal Highlights
| Title | Journal | Authors |
| ACROBEAT (Adaptive CaRdiac cOne BEAm computed Tomography): Towards the next generation of cardiac imaging in the hybrid theatre | Medical Physics | T. Reynolds, O. Dillon, J. Prinable, B. Whelan, P.J. Keall and R. O’Brien |
| Towards improved 3D carotid artery imaging with Adaptive CaRdiac cOne BEAm computed Tomography (ACROBEAT) | Medical Physics | T. Reynolds, O. Dillon, J. Prinable, B. Whelan, P.J. Keall and R. O’Brien |
| Dual cardiac and respiratory gated thoracic imaging via adaptive gantry velocity and projection rate modulation on a linear accelerator: a proof-of-concept simulation study | Medical Physics | T. Reynolds, C. Shieh, P.J. Keall and R. O’Brien |
| Towards patient connected imaging with ACROBEAT: Adaptive CaRdiac cOne BEAm computed Tomography | Physics in Medicine and Biology | T. Reynolds, C. Shieh, P.J. Keall and R. O’Brien |
Associated Awards
2022 Eureka Prize for Outstanding Early Career Researcher: Dr Tess Reynolds.
2018 Best in Physics, American Association of Physicists in Medicine Annual Meeting:
T. Reynolds, C. Shieh, R. O’Brien and P.J. Keall, “ACROBEAT: Adaptive CaRdiac cOne BEAm computed Tomography”, – American Association of Physicists in Medicine Annual Meeting 2018, Nashville, Tennessee, USA.
ACROBEAT In the Media
- University of Sydney coverage of Eureka Prize (2022): https://www.sydney.edu.au/news-opinion/news/2022/09/01/pioneers-recognised-in-australia-s-top-science-prizes.html
- Article on developing cardiac Patient Connected Imaging (2019). https://physicsworld.com/a/acrobeat-mitigates-cardiac-motion-during-imaging/
- The ‘Best in Physics’ e-poster presentation at the American Association of Physicists in Medicine Annual Meeting 2018.https://physicsworld.com/a/aapm-showcases-the-best-in-physics/